Between 60% and 80% of people will experience low back pain at some point in their lives. A high percentage of people will have low back and leg pain caused by a herniated disk.
Lumbar disc herniation
Although a herniated disk can sometimes be very painful, most people feel much better with just a few weeks or months of nonsurgical treatment.
The nerve runs through the leg, and any type of pinched nerve in the lower spine can cause pain to radiate along the path of the nerve through the buttock and down the leg. This type of pain is also called sciatica or a radiculopathy
Anatomy
Your spine is made up of 24 bones, called vertebrae, that are stacked on top of one another. These bones connect to create a canal that protects the spinal cord.
Five vertebrae make up the lower back. This area is called your lumbar spine.
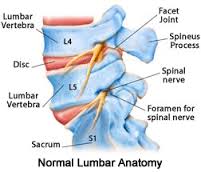
Parts of the lumbar spine
Other parts of your spine include:
Spinal cord and nerves. These "electrical cables" travel through the spinal canal carrying messages between your brain and muscles.
Intervertebral disks. In between your vertebrae are flexible intervertebral disks. They act as shock absorbers when your walk or run.
Intervertebral disks are flat and round, and about a half inch thick. They are made up of two components:
Healthy intervertebral disk (cross-section view).
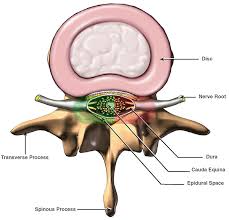
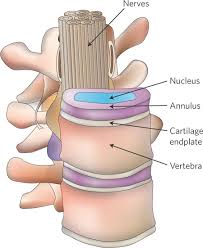
• Annulus fibrosus. This is the tough, flexible outer ring of the disk.
• Nucleus pulposus. This is the soft, jelly-like center of the disk.
Description
A disk begins to herniate when its jelly-like nucleus pushes against its outer ring due to wear and tear or a sudden injury. This pressure against the outer ring may cause lower back pain.
If the disk is very worn or injured, the jelly-like center may squeeze all the way through.
Once the nucleus breaks — or herniates — through the outer ring, pain in the lower back may improve. Sciatic leg pain, however, increases. This is because the jelly-like material inflames the spinal nerves. It may also put pressure on these sensitive spinal nerves, causing pain, numbness, or weakness in one or both legs.
Lumbar Herniated Disc Symptoms
General symptoms typically include one or a combination of the following:
• Leg pain (sciatica), which may occur with or without lower back pain. Typically the leg pain is worse than the lower back pain.
• Numbness, weakness and/or tingling in the leg
• Lower back pain and/or pain in the buttock
• Loss of bladder or bowel control (rare), which may be an indication of a serious medical condition called cauda equina syndrome.
.
The vast majority of disc herniations will occur toward the bottom of the spine at L4- L5 or L5- S1 levels. In addition to typical sciatica symptoms, nerve impingement at these levels can lead to:
• L5 nerve impingement (at the L4 – L5 level) from a herniated disc can cause weakness in extending the big toe and potentially in the ankle (foot drop). Numbness and pain can be felt on top of the foot, and the pain may also radiate into the buttock.
S1 nerve impingement (at the L5 – S1 level) from a herniated disc may cause loss of the ankle reflex and/or weakness in ankle push off (patients cannot do toe rises). Numbness and pain can radiate down to the sole or outsid
Cause
In many cases, a herniated disk is related to the natural aging of your spine.
In children and young adults, disks have a high water content. As we get older, our disks begin to dry out and weaken. The disks begin to shrink and the spaces between the vertebrae get narrower. This normal aging process is called disk degeneration.
Risk Factors
In addition to the gradual wear and tear that comes with aging, other factors can increase the likelihood of a herniated disk. Knowing what puts you at risk for a herniated disk can help you prevent further problems.
Gender. Men between the ages of 30 and 50 are most likely to have a herniated disk.
Improper lifting. Using your back muscles to lift heavy objects, instead of your legs, can cause a herniated disk. Twisting while you lift can also make your back vulnerable. Lifting with your legs, not your back, may protect your spine.
Weight. Being overweight puts added stress on the disks in your lower back.
Repetitive activities that strain your spine. Many jobs are physically demanding. Some require constant lifting, pulling, bending, or twisting. Using safe lifting and movement techniques can help protect your back.
Frequent driving. Staying seated for long periods, plus the vibration from the car engine, can put pressure on your spine and disks.
Sedentary lifestyle. Regular exercise is important in preventing many medical conditions, including a herniated disk.
Smoking. It is believed that smoking lessens oxygen supply to the disk and causes more rapid degeneration.
Medical History and Physical Examination
After discussing your symptoms and medical history, your doctor will examine your spine. During the physical examination, your doctor may conduct the following tests to help determine the cause of your low back pain.
Neurological examination. A physical examination should include a neurological examination to detect weakness or sensory loss. To test muscle weakness, your doctor will assess how you walk on your heels and toes. Your thigh, ankle, and toe strength may also be tested. Your doctor can detect any loss of sensation by checking whether you are numb to light touch in the leg and foot. In addition, your reflexes at the knee and ankle will be tested, and sometimes may be absent.
Straight leg raise (SLR) test. This test is a very accurate predictor of a disk herniation in patients under the age of 35. In this test, you lie on your back and your doctor lifts your affected leg. Your knee stays straight. If you feel pain down your leg and below the knee, you test positive for a herniated disk.
Imaging Tests
To help confirm a diagnosis of herniated disk, your doctor may recommend a magnetic resonance imaging (MRI) scan. This scan can create clear images of soft tissues like intervertebral disks.
Lumbar Herniated Disc Treatments
In most cases, if a patient’s pain is going to get better it will start to do so within about six weeks.
While waiting to see if the symptoms will abate on their own, several non-surgical treatments can help alleviate the pain and facilitate long term healing. The most common herniated disc nonsurgical treatments include:
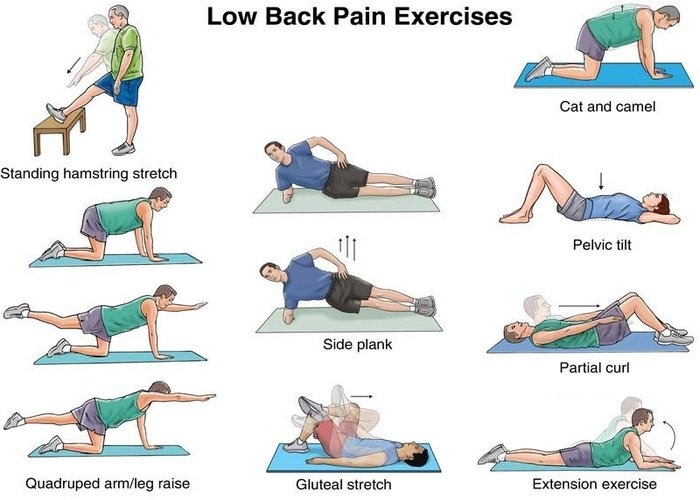
• Physical therapy
•
• Osteopathic/chiropractic manipulation (manual manipulation)
• Heat and/or ice therapy
• Non-steroidal anti-inflammatory drugs (NSAIDs)
• Oral steroids (e.g. prednisone or methyprednisolone)
• An epidural (cortisone) injection
If the pain and other symptoms continue after six weeks, and if the pain is severe, it is reasonable to consider microdiscectomy surgery as an option.
Lumbar Herniated Disc Surgery
Only a small percentage of patients with lumbar disk herniations require surgery. Spine surgery is typically recommended only after a period of nonsurgical treatment has not relieved painful symptoms.
Microdiskectomy. The most common surgical procedure for a herniated disk in the lower back is a lumbar microdiskectomy. Microdisketomy involves removing the herniated part of the disk and any fragments that are putting pressure on the spinal nerve.
Rehabilitation. Most patients do not require formal physical therapy after surgery. After your surgeon evaluates you and confirms that your incision is healed, you may begin a rehabilitation exercise program. A simple walking program 30 minutes each day, along with flexibility exercises for the back and legs, can be done as a home program. If needed, your surgeon will refer you to a physical therapist.